Why do some physiotherapists follow a Cognitive Functional Therapy (CFT) approach when treating chronic pain conditions? What does this mean? Is CFT any better than any other approach? How does it benefit me as a patient?
This blog looks at my experience, as a patient with chronic disabling lower back and sciatic pain, being treated by a physiotherapist following a Cognitive Functional Therapy approach. For me the approach was life changing!
Following a manual handling accident in July 2008 I was left with disabling (and excruciating!) lower back and right sided sciatic pain. I underwent back surgery in December 2009, but I think surgery was carried out too late for me as my sciatic nerve had already been permanently damaged by a prolapsed disc pushing on it for well over a year. I continue to live with daily chronic pain, sometimes severe, and expect to do so for the rest of my life.
During the first four years following the accident I underwent a number of epidural injections, a nerve root block and back surgery. I had a number of physiotherapy episodes of care, was under the care of a rheumatologist and I attended the pain clinic. I was on large quantities of pain killers, including morphine, and suffered badly from side effects. The approximate number of treatments I had, and the number of clinicians involved in my care, are shown in this MindMap.
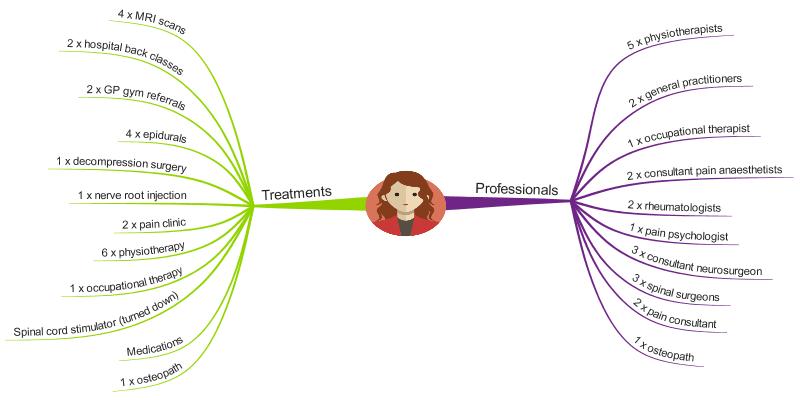
I went back to work very shortly following the accident, despite not being able to sit, stand or walk properly (yes, I know, totally stupid!). I tried hard to deal with my situation the best I could. After back surgery I started on an assessment pathway for a spinal cord stimulator, and at times struggled to cope.
Most of the physiotherapy I received had limited success for me, partly I think due to an over emphasis on core exercises (see my post on core exercises HERE). Although I was being given some basic advice during physiotherapy sessions, I didn’t really understand why my body was constantly in pain, what the triggers for my pain were, and what the realistic likely outcomes were for me. I had developed many maladaptive movements, for example I frequently stood with all my weight on my left foot and leg and I sat leaning on my left side (I was trying to alleviate the pain on my right side). I didn’t really understand pain management, and I simply didn’t know how to move my pain situation further forward, despite my best endeavours to do so.
Whilst on the very lengthy assessment pathway for a spinal cord stimulator I asked my rheumatologist if a further episode of physiotherapy care might help address the severe difficulties I was having with pain when sitting. The resultant physiotherapy input, carried out just over four years after my accident, proved to be life changing for me. I genuinely wish I’d been able to receive it earlier. Matt Low (@MattLowPT) was the physiotherapist (then an extended scope physiotherapist and now a consultant physiotherapist) and the episode of care followed what I now understand to be a Cognitive Functional Therapy approach.
Because the physiotherapy sessions with Matt were so life changing and important to me, I can still remember quite a lot about what happened, but please bear in mind throughout this post that I am reflecting mainly on an episode of care that took place over 5 years ago, so I may well get some details wrong. I have recently been re-referred back to Matt as I needed some additional professional input, and so I will also describe some elements of my most recent episode of care, which also seems to broadly follow the CFT approach.
What os Cognitive Functional Therapy?
Professor Peter O’Sullivan and his research team devised Cognitive Functional Therapy to better support patients with disabling lower back pain. (Peter is a Specialist Musculoskeletal Physiotherapist and a Professor of Musculoskeletal Physiotherapy at Curtin University in Australia.)
I don’t intend to write in detail about the CFT approach, as that is well explained in the article you can access *HERE*, and by many other articles available on the Internet. Just Google ‘Cognitive Functional Therapy’. I don’t pretend to be a medical practitioner and so my explanations are more from a patient’s perspective, and I apologise in advance if I haven’t quite got my explanations around the CFT process quite right – happy for anyone to point out what might need changing!
Cognitive Functional Therapy is divided into the following three main areas:
Making sense of the pain
Helping the patient understand better, and make more sense of, their pain in their own personal context. This includes consideration of the many different factors which affect and contribute to pain. Factors may be physical, social, emotional, life style or health-related. They may also include psychological factors, for example the patient’s pain beliefs, pain hyper-vigilance and pain avoidance. Each patient has their own life context and each patient has their own pain story.
Pain management through functional analysis

Supporting the patient to develop effective pain management strategies for their own particular physiology and context. This includes physical observations of pain-provoking functional behaviours, consideration of the patient’s sensory profile in terms of hyperalgesia and provocation of pain, and whether the patient has any muscle deconditioning. It includes consideration of pain characteristics and maladaptive movement and lifestyle behaviours.
Negative thoughts about pain might be challenged and any emotional responses to pain may be discussed and considered. Patients are encouraged to consider and set goals that are important to them to achieve. They are supported to experiment with different body postures and movements in order to lower pain levels, and relaxation techniques may be taught. Patients may be taught how to gradually challenge and improve some physical contributors of their pain, for example leaning forward.
Supporting a healthy lifestyle
Supporting and encouraging the patient to adopt a healthy lifestyle, despite pain.
My Cognitive Functional Therapy Experience
Albeit over four years after my accident, I was fortunate to have been given a reasonable number of sessions of physiotherapy based on a CFT approach, over a period of 9 months. I have recently received a few additional sessions, which have served as a ‘top up’.
Looking back at the three main CFT areas described above, the therapy I received covered most of the elements described within each section. Rather than give a blow by blow account of the therapy I received, and how it followed these areas, I’ve decided to pick out 5 aspects which I think illustrate why Cognitive Functional Therapy worked so well for me and how this care differed from my previous physiotherapy care.
I have included in italics some excerpts from notes I wrote at the relevant time. I write quite detailed notes for most physiotherapy sessions I attend in order to summarise the work I have been doing in between sessions and to raise questions I am hoping to get answers to. I often just hand the notes over to the treating physiotherapist to read so that they have a quick summary of my thoughts at the beginning of the session.
Pain education and making sense of my pain

It’s hard to believe that after four years of living with severe pain, and after a range of inputs from medical professionals, including physiotherapists and the pain clinic, that actually my understanding of pain, in particular my pain, and how to manage it beyond taking medications was probably in real terms negligible!
I can remember the CFT physiotherapy sessions with Matt not feeling time pressured, and I can remember feeling that he had a genuine interest in both my pain story and me as a person. Through the sessions he got to know me as an individual and I felt valued. I felt I was able to disclose anything about my pain, including the irrational fears and emotions it was causing me to experience. Throughout the sessions Matt used sensitive non-judgemental questioning, and carefully prompted me when needed. This type of questioning probably wasn’t too much different to other physiotherapists that had treated me, although I think Matt was more skilled at it, but I think it was what he then did with what I was saying that was so very valuable to me, and so different.
Matt recognised that my understanding of my pain was pretty low and built on the basic understanding I had with verbal, pictorial and physical explanations and with suggestions for reading outside of the therapy sessions (these suggestions for external reading were really important, particularly for my long-term continuation of learning). Matt revisited and extended my understanding throughout the episode of care, and again during my most recent episode of care.
‘Bought the book you suggested – that was a turning point for me and I’m very grateful to you for telling me about it. I have a much better understanding of what is going on now.’
Most importantly Matt took me from thinking that the pain was basically unidimensional (ie there was something physically wrong with my back at that moment in time and it was therefore responding with pain), to an understanding that pain is much more complex and affected by many different things, including what I do during the day and my emotions. This was hugely important for me as it opened the door to me understanding what in simple terms might be feeding into my pain, and even more importantly what I could try and do to self-manage the pain. No other medical professional had attempted to do this (at least not from my recollections, and so if they did they clearly weren’t successful!). I cannot over-emphasise how important this understanding was to me in terms of being able to learn to pro-actively self-manage my pain situation better. I have written a blog about the pain management that I developed with Matt, which can be accessed by clicking HERE.
‘Interestingly there were some things that you taught me about my condition that I had been told before, but you were able to impart the knowledge and understanding in just the right way for me. You listened to what I said and moved my understanding forward in a very sensitive way.’
I’ve often wondered if it mattered what type of healthcare professional worked with me on this understanding of pain, but certainly for me I think it was important that this ‘pain education’ was undertaken by a physiotherapist. I can quite see an argument that different clinicians could have performed this role, and maybe it was a waste of a physiotherapists time, but actually I needed to understand how the pain mechanisms were likely to be working for my particular physiological and neurological condition, and for that I needed a physiotherapist. I needed to be able to ask detailed and searching questions about my physiology that were firmly within the physiotherapists scope, and out of the scope of say an occupational therapist, a pain psychologist or pain nurse. I needed the reassurance that I could physically do more than I was doing without causing further harm. I needed to understand physically what I could do to help my situation. I needed to understand about the maladaptive movement behaviours I had developed, and how to address them. It was the mix of the understanding of pain mechanisms and the understanding of my own physiological and neurological condition that was so important for me. One without the other or being delivered by two or more different professionals, particularly in a non-joined up manner, would not have worked nearly so well.
‘I can’t know what will happen in terms of a spinal cord stimulator, or indeed anything else that may happen down the line, but I do know that however difficult my condition may or may not be at any one time, I would be in a much worse place without the knowledge and understanding that you imparted to me.’
Maladaptive movement behaviours

Matt was very skilled at observing my pain behaviours and the way I held my body, describing to me what I was doing and then suggesting and working with me on ways forward.
For example, because my pain is predominantly right sided I had spent the first four years following my accident putting my weight on my left side in order not to cause further pain on the right. I must have looked very lop sided, as when sitting I tended to lean on my left hand with my right side slightly raised, and when standing I would basically be standing on my left leg with my right leg just there for balance! I had absolutely no idea I was doing this, but I can appreciate that this really wasn’t the best thing to do for my long term physical health. It took a number of weeks, and some hard work, to resolve, but Matt was able to resolve this with me, and in general I now stand in a more balanced position (or at least I think I do!).
‘Stood on one leg as much as possible. I can understand why I had been subconsciously not. This increased numbness and pain, particularly in foot and hip/thigh, and at times made it very painful to walk. Also caused increased back pain/spasms.’
Matt worked with me on a number of maladaptive behaviours that in the main I had not even appreciated were occurring. One of the down sides of this is that I no longer have any visible signs of my condition, which means I experience an additional range of problems associated with having a hidden disability. Looking ‘normal’ but needing someone to help manage my heavy briefcase and luggage at train stations has needed a bit of work, including on my emotions!
‘I feel I suffer from a ‘hidden disability’ as outwardly there appears to be nothing wrong with me. For example, I still find it difficult to ask for help lifting what to other people must seem relatively small bags on say trains. I usually tell people I have had back surgery, and everyone I have asked has been really happy to help, but I find it difficult to actually ask for that help. I sometimes think if I looked as though there was a real problem then people would offer rather than me ask; that would be so much easier.’
I have written a post about my difficulties about having a hidden disability, called “‘The Invisible Barrier of Perception’ that hinders self management”, which can be accessed HERE.
My recollection is that no other physiotherapist had previously tried to resolve any of my maladaptive pain behaviours. Although integral to the CFT approach, working on these pain behaviours could have been undertaken as a discrete piece of work by my other physiotherapists, but it wasn’t. I think these pain behaviours were important to resolve, particularly for my long term physical health.
Experimenting with different body postures and movements
Another very important aspect of Cognitive Functional Therapy for me was being taught by Matt to step outside of ‘universal advice’ and to learn to listen to my body and put in place things that worked for me, rather than things that were ‘supposed to work’ for people with back problems . For example, just after my accident I was advised by my physiotherapist to buy a lumbar roll and to sit on wedged cushions, with a back support and to sit up straight. This advice was reinforced by ‘public opinion’ and also by the marketing associated with back support devices. I can’t remember if other physiotherapists advised the same or not, but certainly none of them suggested I should throw that piece of learning out of the window and look at what my body actually needed to manage my personal pain situation.
Sitting has been, and continues to be, a huge problem for me. It wasn’t until Matt challenged my misconceptions of how I should be sitting and what I should be sitting on that I started to make any headway in terms of easing my situation. Matt taught me to try different body positions and postures, to try softer cushions and to try different types of chair. Most of all he taught me to listen to my body and experiment. I now know that it is best for me to sit on a very soft cushion (I use a particular type of wheelchair cushion), not to sit on a chair with any type of lumbar support (my back hurts in places and the lumbar support sticks into it and aggravates it), and I certainly wouldn’t use a lumbar roll which for me would hurt. Sitting up straight is probably the most difficult position for my back and sciatic nerve, and although I have no choice sometimes when working, when I do have a choice I avoid it as much as possible.
Tried the ‘slouch’ position when sitting. Can’t believe I had so rigidly avoided this before.’
It is regrettable that immediately following my accident I was taught by a physiotherapist to adopt ‘universal advice’ about sitting, rather than them working with me to look at how I could learn to sit again with as little pain as possible. Sitting is hard to avoid, especially if you experience increased pain standing still or walking as well, and so being helped to sit in a more comfortable way through the CFT approach was hugely important to me.
Reducing pain provocation

Part of the Cognitive Functional Therapy approach is for the physiotherapist to listen to the patient’s story, or a description of some aspects of it, pick out the salient points, apply clinical reasoning to make a hypothesis, reflect this back to the patient in order to discuss and work together to try to move the patients physical and pain situation forward.
For example, when I was describing to Matt what was causing increased pain in my day to day life, he was able to pick out from the wide range of examples I was giving that I was describing a number of different instances when my body was in a sustained position. For example, pain increased when standing still, when sitting still and when leaning forwards and to the right for a while, when walking at a steady pace for a while. He put forward a hypothesis that sustained movements were provoking pain for me, and suggested that I try varying my pace when walking and to avoid other sustained movements the best I can. Once alerted to this possibility I was able to think about how I could avoid such situations, and this has helped. For example, when waiting for a train I walk up and down the platform instead of standing in one spot (no one else seems to do this, so I must look very strange, but it helps me so I do it anyway). When walking to places I try to vary the pace I’m walking at and when sitting I try to adjust the position I’m in as much as possible.
As mentioned before, I often write up to a page of bulleted notes before attending a physiotherapist appointment, which I usually give to the physiotherapist at the beginning of the session. Other physiotherapists have just read them and picked up on one or two points. Matt goes through them carefully picking out any connections he can find between the points I am making, and what he knows about my condition already, and will reflect back to me any thoughts he has based on his clinical reading of my descriptions, and on any hypothesis he may be forming. I can’t remember any other physiotherapist doing this, but I have found it hugely valuable. Apart from any resultant benefit in treatment, knowing that my input and thoughts are valued in this way supports the ‘working together’ framework that CFT is based on.
Challenging and supporting negative thoughts and emotional responses
Experiencing a life changing accident, and then embarking on a life of disability and chronic pain is fundamentally traumatic! Different people react in different ways, partly based on their life experiences, their resilience, their emotional and mental health, and their basic individual makeup. I brought into my chronic pain experience a high level of resilience, some vulnerabilities including a slightly anxious disposition, a positive outlook on life and reasonably stable mental and emotional health. I have been fortunate that I haven’t become depressed through the experience, which is so very common in these circumstances and so very understandable.
I have recently found the following description of my emotions, which I wrote just over 3 years after my accident and around 9 months before starting my work with Matt. It describes quite well the emotions that I brought into the CFT sessions with Matt, and with which he needed to support me.
‘I have found it very difficult emotionally to come to terms with my situation. I have had to live with constant pain, sometimes severe, over the last 3 years, and I have lost my career through it. In many ways the biggest emotional impact for me has been, and remains, the thought of facing the possibility of say another 30 years in constant pain, some of that severe. It is usually when I talk about the future of my life in pain with doctors or physiotherapists that I dissolve into tears or fight back tears with them.
I have found it difficult to stop fighting against my physical situation in order to work full time, and accept that if I want to live a life without significant severe pain that I actually have to totally change my life style and work plans and work part time with much of that work taking place at home and not in a workplace. This has been enormously difficult for me, the main help along the way has been the severe pain which has occurred when I have tried to work outside from home and has strongly reminded me that I can’t cope with a life of frequent severe pain and everything that comes with it in terms of strong painkillers and their side effects and lack of sleep. Even now, a good dose of severe pain reminds me that I have to continue to alter my work and life style.’
If I’m honest I can’t remember any specific occasions Matt supported me with my thoughts and emotions around pain, the sessions after all weren’t counselling sessions, but I do remember feeling hugely supported throughout. Throughout the sessions Matt sensitively challenged my thoughts and feelings regarding my situation, and at the same time supported me learning and developing pain management skills such that I felt better able to deal with my situation and have more hope for my future life with pain. Although this process undoubtedly helped my overall situation, it did inevitably cause my emotions to reactively swing wildly at times, particularly in between sessions, which was sometimes hard to deal with.
‘There are times I’m still really struggling, and I just cannot seem to stop the dips into struggling. I assume this is just part of living with a chronic pain condition and I shouldn’t beat myself up about it?’
Although I’m guessing a pain psychologist could have taken me through addressing the negative thoughts and emotions I was experiencing living with chronic pain, I think having a holistic approach where I was being taught pain management skills at the same time, and by the same therapist, worked better for me. After all the most prominent difficulty for me at the time, as described in my contemporaneous writing above, was the thought of living for the next 30 years or so in chronic pain, often severe. Addressing that negative thought and emotion was bound to be much easier when combined with developing pain management skills, such that I could see that I could make a difference to my situation going forward. I have no recollection of any of my other physiotherapists taking this holistic approach and strongly supporting the emotional side of living in chronic pain, I wish they had.
‘It is hard for me to adequately describe the importance to me of what I learnt from you about my nerve pain condition and how best to manage it, and therefore how best to make the most of my life. I’m not in any way trying to pretend that I now have full control of my condition, nor that it doesn’t still have a huge impact on my life, but there is no doubt that I have a much larger pain management toolbox than I had, and that I have a more confident and optimistic outlook to the rest of my life thanks to you. I am under no illusions that without your professional care that I would be in a quite different place, both physically and emotionally, now.’
When I returned to Matt for a further physiotherapy episode of care in 2018 I wrote in my notes,
‘Matt, first of all I would like to say a huge thank you for the work you did with me in 2013. I truly believe you changed my life. Sounds dramatic, but I believe you did.’
…. and that’s how I feel about Cognitive Functional Therapy
…. life changing!
Tina
@livingwellpain
www.livingwellpain.net











Beautiful Tina, thank you
Lloyd .a physio 🙏❤️✌️
Thanks Lloyd, very much appreciated.
Tina
Good for you Tina-a truly candid description of your journey with chronic pain. It only serves to reinforce the value of those sessions where I “ just listen and talk with my patients” never taking off a piece of Corning or laying so much as a hand on them. Thankyou
Just started on my journey of pain and the mind. I would be interested to know.. what was the book that was recommended to you ?
Hi Lisa
The book was called ‘Explain Pain’. Worth a read, although not cheap if I remember rightly.
Best wishes with your journey 😊😊😊
Tina